 Pain Management Coding Updates for 2023
Pain Management Coding Updates for 2023
CMS introduced new CPT codes for Chronic Pain Management (CPM) services in the 2023 Medicare Physician Fee Schedule Final Rule as part of...
 Pain Management Coding Updates for 2023
Pain Management Coding Updates for 2023
CMS introduced new CPT codes for Chronic Pain Management (CPM) services in the 2023 Medicare Physician Fee Schedule Final Rule as part of...
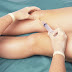 Arthrocentesis CPT Codes 20610, 20605, 20600 knee Injection
Arthrocentesis CPT Codes 20610, 20605, 20600 knee Injection
The joint effusion or the accumulation of intraarticular fluid can be caused by a variety of medical conditions, injuries, and infections...
 CPT Codes for Ultrasound of Liver and Gallbladder 76705, 76700
CPT Codes for Ultrasound of Liver and Gallbladder 76705, 76700
One CPT code can be used for multiple organs or anatomic sites in a Radiology facility. Radiology CPT codes fall into two categories: 700...
 Acute Respiratory Failure with Hypoxia ICD 10 Codes
Acute Respiratory Failure with Hypoxia ICD 10 Codes
Respiratory failure is a syndrome that occurs when the respiratory system's gas exchange functions - oxygenation and carbon dioxide e...
 Meniscus Tear Right & Left Knee ICD-10 Codes
Meniscus Tear Right & Left Knee ICD-10 Codes
Meniscus tear is a tear in the cartilage of the knee is one of most common knee injuries. The meniscus is a piece of cartilage that betwe...
 Laceration Repair CPT Codes 12001, 12002, 12011, 12031, 12032
Laceration Repair CPT Codes 12001, 12002, 12011, 12031, 12032
Skin laceration repair is an important skill in family medicine. Lacerations are common in urgent care and emergency room settings. In th...